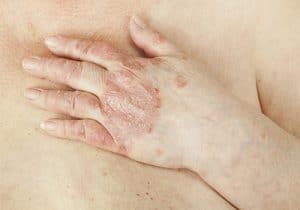
Psoriatic Arthritis
Psoriatic arthritis is a form of arthritis that affects some people who have psoriasis- a condition that features red patches of skin topped with silvery scales. Most people develop psoriasis first and are later diagnosed with psoriatic arthritis but the joint problems can sometimes begin before skin lesions appear.
Joint pain stiffness and swelling or the main symptoms of psoriatic arthritis. They can affect any part of your body including your fingertips and spine and can range from relatively mild to severe in both psoriasis and psoriatic arthritis.
Treatment
Without treatment psoriatic arthritis may cause disability. Your doctor may recommend medication to help reduce inflammation in your joints. In severe cases, the doctor may recommend surgery that can improve your joint movement.
To treat skin symptoms, topical treatments will be recommended that you apply directly to your skin to reduce itching and scaling.
Advance Explanation
A patient, previously misdiagnosed, with common elbow pain was referred to RARA. After a thorough examination of a patient’s history and careful diagnosis of the elbow, the cause of the pain was determined as lateral epicondylitis, commonly known as ‘Tennis elbow’. Further detailed examinations revealed that the patient was suffering from enthesitis ( inflammation of the entheses, the sites where tendons or ligaments insert into the bone), dactylitis (sausage digit, because it looks like a sausage), pitting of a couple of fingernails, and some psoriasis in the Umbilicus (belly button).
Careful examination of the patient’s history and proper diagnosis resulted in a change of treatment from a localized/isolated tennis elbow to a diagnosis of Psoriatic arthritis. Psoriatic arthritis occurs in various forms. It can look similar to rheumatoid arthritis (RA), involving the spine in a way similar to ankylosing spondylitis (inflammation of the spine), and can be associated with non-musculoskeletal issues such as sores in the mouth and inflammation in the eye. Though there is a possibility of having Rheumatoid Arthritis in combination with, unrelated to psoriasis.
This case- study shows how the pattern of joint involvement can lead to a correct but elusive diagnosis. Precise questioning by experienced physicians and a comprehensive assessment of joint involvement patterns can help to reach an accurate diagnosis. Similar cases such as Psoriatic skin/nail changes, may predate the joint symptoms, or even follow the joint symptoms for years. It is important to understand that X-rays and labs can assist in the diagnosis, but will not be helpful for “uninitiated/inexperienced” observers. Psoriatic arthritis can be primarily diagnosed through investigation of the patient’s history, physical examination, and the experience of the physician. The lab and x- rays are only ancillary.
A patient with a positive Rheumatoid factor does not necessarily mean they have RA and not psoriatic arthritis. Patients suffering from chronic illness, characterized by periods of relative improvement and then periods of flare-ups or worsening need specific treatment. We aim to control the number of flares, the severity of the baseline level of inflammation, discomfort, and disability, and to lessen the severity and the duration of flares.
We place the problem into prolonged remission with drugs such as Methotrexate, and other DMARD (Disease Modifying Anti-rheumatic Drugs) and/or Biologic modifiers, such as Remicade, Humira, and Enbrel, just to mention a few. Because of potential side effects, we tend to use less often, the class of drugs known as Non-steroidal anti-inflammatory drugs (NSAIDs). The treatment has improved by leaps and bounds since my initial period as a physician.
